 Temple University agreed to pay $100,000 to settle claims that it overbilled Medicare and Medicaid for neurology services. The settlement agreement covers alleged overbilling for services provided by Temple University physicians at the university’s own facilities and at Frankford Hospital. According to the government, the university submitted claims to Medicare and Medicaid using codes that resulted in higher payments for services than the codes that should have been used based on the medical documentation supporting the services. Using a higher billing code than the documentation supports is known as “upcoding.” After reviewing the government’s allegations and the underlying documentation, the university agreed that the coding was not accurate. Upcoding is just one type of billing practice that results in Medicare and Medicaid paying more for services than they should. Healthcare providers can be charged with upcoding when they use the wrong code or when the documentation supporting the claim for reimbursement is inadequate to justify the code that was used. Other improper billing practices include “unbundling” and “double billing.” Unbundling involves charging separately for services and procedures that should be billed under a single billing code. Double-billing occurs when a healthcare provider bills both government programs and either private insurers or patients. Upcoding, unbundling, and other types of improper billing practices are serious violations of the federal False Claims Act. They can result in treble damages and penalties of $11,000 for each claim submitted to the government. But these billing practices are often difficult to detect. That is why the government pays whistleblower rewards to individuals who come forward with evidence of improper, false or fraudulent claims. Under the federal False Claims Act, an individual who helps the government stop Medicare and Medicaid fraud and abuse is entitled to a whistleblower reward of between 15% and 30% of the amount the government recovers. These whistleblower rewards can amount to tens of thousands of dollars, hundreds of thousands of dollars, and in some cases millions of dollars. If you are aware of false or improper claims submitted to Medicare or Medicaid, then you should consult with an experienced whistleblower attorney. You may be entitled to a substantial whistleblower reward and legal protections under the False Claims Act. To arrange a free and confidential consultation with an experienced whistleblower attorney, call John Howley, Esq. at (212) 601-2728 or click here to reach our offices via email. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.
0 Comments
 One of the great tragedies of Medicare fraud is when the corporation that received millions of dollars settles the fraud case by paying back money, while the employees who were asked to sign false documents end up in prison. It happens all the time. A physical therapist is asked to authorize more therapy than the patient really needs. An EMT who transports patients in ambulances to dialysis treatment is asked not to indicate on the trip report that the patient was in a wheelchair or able to walk. A visiting nurse is asked to submit time sheets for more time than was actually spent with the patient. The employer uses these documents to submit millions of dollars in false claims to Medicare. When they get caught – and at some point they always get caught – the employer pays back the money, and the employees go to prison. In a recent case, a registered nurse pleaded guilty to home health fraud after government investigators discovered that she had signed false documents for a home health care company. The nurse admitted that she created nursing visit notes to justify home health care services that the patients did not really require. She also admitted that she signed nursing visit notes for home visits, when the visits were actually made by other individuals who were not licensed. The employer used these types of false records from this nurse and others to submit $24 million in false claims to Medicare for home health care services. The nurse now faces up to ten years in prison and a fine of up to a $250,000. If the nurse had contacted an experienced whistleblower attorney, she could have protected herself and earned a substantial reward. Under the federal False Claims Act, individuals who help the government stop Medicare fraud are entitled to a whistleblower reward of between 15% and 30% of the amount the government recovers. For example, if this nurse had helped the government collect $24 million from the home health care company, she would have been entitled to a whistleblower reward of between $3.6 million and $7.2 million. Instead, she is facing the possibility of a very long prison sentence. Do not go to prison for your employer’s fraud. If you are aware that your employer is creating false documents, then you should consult with an experienced whistleblower attorney immediately. You may be entitled to legal protections and a substantial reward under the False Claims Act. To arrange a free and confidential consultation with an experienced whistleblower attorney, call John Howley, Esq. at (212) 601-2728 or click here to reach our office by email. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.  One of the most common forms of ambulance fraud is billing Medicare for non-emergency transportation of patients who are not bed-confined or who are able to travel in another form of transportation. This type of ambulance fraud often occurs when transporting patients to dialysis centers. Individuals who help the government stop this type of fraud are entitled to very substantial whistleblower rewards under the federal False Claims Act. Recently, the president of a local rescue squad in Virginia was caught submitting false claims to Medicare for medically unnecessary, non-emergency ambulance transports. Over a five-year period, the false claims added up to more than $1.6 million. Under the false claims act, the government may recover three times the amount it paid plus $11,000 per claim. In a case involving $1.6 million in false claims, the government can recover more than $5 million. The potential whistleblower reward in this type of case is between 15% and 30% of the amount recovered by the government. In a case involving $1.6 million in false claims, that means a potential whistleblower reward of between $750,000 and $1.5 million. In order to receive Medicare reimbursement for non-emergency ambulance transports, the patient must be bed-confined or have a medical condition that renders ambulance transport necessary. The ambulance company must obtain a Physician Certification Statement (PCS) stating that the patient requires ambulance transportation. But the existence of a signed PCS does not automatically qualify the patient for non-emergency ambulance transportation reimbursement from Medicare. If the PCS is false – that is, if the patient is not bed-confined and their medical condition would allow them to be transported in a wheelchair van – then any claims submitted to Medicare for non-emergency ambulance transport services are considered false claims. The government has a hard time identifying this type of fraud, because it cannot see the condition of the patients when they are picked up for transport. That is why most whistleblower rewards for ambulance fraud go to EMTs, drivers, medical billers, and other individuals who work for the ambulance companies. For example, an EMT may notice that most of the patients transported by his or her ambulance company are able to walk or sit in a wheelchair when they are picked up for scheduled ambulance transportation. Or a medical biller may notice that patients transported by ambulance do not have current or valid Physician Certification Statements (PCS) in their files. In some ambulance companies, employees are asked not to note the patient’s condition on trip reports. Or medical billers are asked to disregard the dates on Physician Certification Statements when submitting claims. And in some cases, employees are asked to create false documents to support their employer’s Medicare claims. This puts the employee in a very dangerous position. When the government discovers the false claims (and, at some point, it will), anyone who participated in submitting the false claims could end up in prison. Remember the president of the local rescue squad in Virginia who submitted $1.6 million in false claims to Medicare for ambulance transport services? He was not the only one targeted by prosecutors. An employee of the rescue squad who went along with the fraud was sentenced to two years of probation and ordered to pay more than $750,000 in restitution to Medicare. Do not risk criminal charges by turning a blind eye to your employer’s ambulance fraud. If you are aware of false claims submitted to Medicare for ambulance transport services, then you should consult with a whistleblower attorney immediately. You may be entitled to a significant whistleblower reward and legal protections. The consultation is free and completely confidential. An experienced whistleblower attorney will listen to you and answer your questions. If you have a case, you will be represented on a contingency fee basis -- no attorneys’ fees are charged unless you win. To arrange a free and confidential consultation with an experienced whistleblower attorney, call John Howley, Esq. at (212) 601-2728 or click here to reach our offices via email. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules. 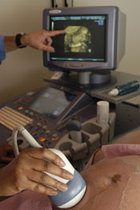 A former revenue manager and coding compliance officer for a radiology practice will receive a whistleblower reward of between $345,000 and $575,000 for helping the government uncover double billing of Medicare and Medicaid by his former employer and one of its clients. The whistleblower went to the government with evidence that Children’s Physician Services of South Texas had billed and received payment for professional services provided by a radiology practice and, without disclosing the payments, directed the radiology practice to bill and receive payment for the same professional services. Here’s how the fraud worked. Technicians working for Children’s Physician Services took genetic ultrasounds of patients and sent the resulting images to Radiology Associates for reading and interpretation by a physician. Children’s Physician Services then billed Medicare and Medicaid for both the taking of the ultrasound and the reading and interpretation of the ultrasound image. When Radiology Associates billed for its professional services, that resulted in double billing of Medicare and Medicaid for the reading and interpretation of the ultrasound image. At some point, the government alleged, Radiology Associates learned of the double billing but continued to bill Medicare and Medicaid anyway. A former coding manager at Radiology Associates ended the fraud – which involved thousands of ultrasound images over a five-year period – by commencing a qui tam or whistleblower lawsuit under the False Claims Act. The lawsuit was filed “under seal” and disclosed only to local prosecutors. The prosecutors then conducted an investigation and decided to join in the lawsuit. Children’s Physician Services and Radiology Associates agreed to settle the lawsuit by paying a total of $2.3 million. Under the False Claims Act, the former coding manager will receive between 15% and 25% of that amount as his whistleblower reward, for a total reward of between $345,000 and $575,000. If you are aware of false claims submitted to Medicare or Medicaid, then you should consult with an experienced whistleblower attorney to find out if you may be entitled to a whistleblower reward and legal protections. To arrange a free and confidential consultation with an experienced whistleblower attorney, call John Howley, Esq. at (212) 601-2728 or click here to reach our office via email. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.  A former nursing home employee will receive a $405,000 whistleblower reward for helping the government uncover false claims submitted to Medicare and Medicaid for physical, occupational, and speech therapy services. Doug Ottinger, a former administrative assistant at Grace Healthcare, went to the government with evidence that his former employer had billed Medicare and Medicaid for physical, occupational, and speech therapy services that were not medically necessary. The government investigated the allegations and decided to join in a lawsuit against the nursing home management company. The lawsuit alleged that Grace pressured therapists to increase the amount of therapy provided to patients in order to meet targets for Medicare revenue. Those revenue targets, the government alleged, were established without regard to an individual patient’s need for therapy. The company agreed to settle the case by paying $2.7 million. Mr. Ottinger will receive $405,000 of that amount as his whistleblower reward. The lawsuit was filed under the qui tam or whistleblower provisions of the federal False Claims Act. The qui tam provisions allow an individual citizen to bring a whistleblower lawsuit on behalf of the government and share in any recovery. In this case, the former employee’s lawsuit was filed “under seal” (in secret) and disclosed only to the government. After investigating his allegations, the government decided to intervene or join in the lawsuit. The government then took the lead in the lawsuit against his former employer and negotiated the settlement. If you are aware that your current or former employer has submitted claims to Medicare or Medicaid for products or services that were not necessary or not actually provided, then you should consult with an experienced Medicare whistleblower attorney immediately. You may be entitled to a substantial whistleblower reward and legal protections. To arrange for a free and confidential consultation, call John Howley, Esq. at (212) 601-2728 or click here to reach our offices via email. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.  Two former pharmaceutical sales representatives will share a $4.4 million whistleblower reward for reporting their former employer’s off-label promotion of a drug to treat weight loss in AIDS patients. Michael McKeen and Courtney Combs started a qui tam or whistleblower lawsuit against their former employer, Par Pharmaceuticals, under the False Claims Act. They alleged that Par Pharmaceuticals, a generic drug company, promoted Megace® ES for uses that were not approved by the Food and Drug Administration (FDA) and not covered by federal healthcare programs. While the FDA approved Megace® ES to treat dangerous weight loss in AIDS patients, Par actively promoted the drug for cachexia or weight loss suffered by elderly patients with no diagnosis of AIDS. This was not an FDA-approved use, nor was this use covered by Medicare or Medicaid. Under the federal False Claims Act, sales representatives and other individuals with knowledge of off-label marketing may start a whistleblower or qui tam lawsuit on behalf of the government and share in any recovery. The qui tam lawsuit is filed “under seal” (in secret) and provided only to the U.S. Attorney. The U.S. Attorney then must conduct an investigation into the claims in the sealed lawsuit. In this case, the government found that “Par deliberately and improperly targeted elderly patients with weight loss residing in nursing homes, regardless of whether such patients suffered from AIDS or any other medically accepted indication.” The government therefore intervened or joined in the qui tam lawsuit. After the government intervened, Par agreed to pay $22.5 million to settle the qui tam lawsuit. The company admitted that it promoted Megace® ES for older patients without AIDS, and that it instructed its sales staff to falsely claim that the drug was more effective than other products. The settlement agreement provides that the two whistleblowers will receive $4.4 million as their whistleblower reward. Par will also pay their attorneys’ fees. If you are aware of off-label promotion of pharmaceuticals, or other false and fraudulent marketing practices involving prescription drugs, then you should consult with an experienced whistleblower attorney immediately. You may be entitled to a significant whistleblower reward and legal protections. The consultation is completely free and confidential. No attorneys’ fees are charged unless your lawsuit is successful. To arrange a free and confidential consultation with an experienced whistleblower attorney, call John Howley, Esq. at (212) 601-2728 or click here to reach our offices via email. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.  Therapists who once worked at a Virginia nursing home will receive a whistleblower reward of $122,500 for helping the government recover $700,000 in a Medicare fraud case against their former employer. The therapists went to the government with evidence that their former employer, Fairfax Nursing Center, billed Medicare for physical, occupational, and speech therapy services that were excessive or medically unnecessary. Their claims were filed in a qui tam lawsuit under the whistleblower provisions of the False Claims Act. Under the federal False Claims Act, individual citizens may bring claims on behalf of the government and share in any recovery. The qui tam lawsuit was initially filed “under seal” (in secret), while the government conducted an investigation. After investigating the claims, the government joined the lawsuit and accused the nursing home of billing Medicare for excessive, medically unnecessary, and otherwise non-reimbursable physical, occupational, and speech therapy services. The government alleged that services billed to Medicare were not necessary for treatment of the patients’ conditions. In some instances, treatment was provided or extended solely for the purpose of billing Medicare. The nursing home agreed to settle the allegations of Medicare fraud by paying $700,000. Under the False Claims Act, the therapists who brought the qui tam lawsuit are entitled to a whistleblower reward of between 15% and 25% of the amount the government actually collects. In this case, the therapists will receive a whistleblower reward of $122,500. Is your current or former employer creating false treatment records or submitting false claims to Medicare? If so, then you should consult with an experienced whistleblower attorney. You may be entitled to legal protections and a whistleblower reward. To find out if you may be entitled to a whistleblower reward, contact John Howley, Esq. at (212) 601-2728 or click here to reach us via email. The consultation is completely free and confidential. No attorneys’ fees are charged unless your case is successful. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.  When prosecutors indicted the owner of a dental practice for Medicaid fraud, they also indicted his office manager, billing manager, and four dentists employed by the practice as co-conspirators in the fraud. Stephen Beukas is a dentist and former owner of New Jersey Mobile Dental Practice, P.A. (”NJ Mobile”). Dentists working for NJ Mobile provided on-site dental treatment to patients at nursing homes, assisted living facilities, adult day care facilities, and private homes. The government alleges that NJ Mobile submitted more than $5 million in false claims to Medicaid by:
As is typical in dental fraud cases, the government did not just arrest the dentist who owned the practice. The government also indicted the office manager, billing manager, and other employees as co-conspirators for going along with the fraud. These employees now face felony fraud charges that could result in long prison sentences and hefty financial penalties. It is too early to tell whether the dental office employees were innocent rubes or willing co-conspirators. But if they knew that false claims were being submitted to Medicaid, they had a number of options that might have avoided the criminal charges they now face. One option was to consult with an experienced whistleblower attorney about the rewards and legal protections available under the state and federal False Claims Acts. Under the federal False Claims Act, an individual citizen may bring a qui tam lawsuit on behalf of the government and share in any recovery. The lawsuit is initially filed “under seal” (in secret), and the evidence is provided only to the prosecutor. The prosecutor then investigates the case and decides whether to take it on. The whistleblower who brings the case is entitled to a reward of between 15% and 30% of the amount recovered. They are also entitled to legal protections against retaliation. The amount of the whistleblower reward depends on the amount actually recovered by the government. In this case, if the government recovered $5 million, then the whistleblower reward would be between $750,000 and $1.5 million. Do not go to prison for your employer’s fraud. If you know that false claims are being submitted to Medicare or Medicaid, consult with an experienced whistleblower attorney immediately to protect your rights, your livelihood, and your freedom. The consultation is free and confidential. No attorneys’ fees are charged unless you win. To arrange a free consultation with an experienced whistleblower attorney, call John Howley, Esq. at (212) 601-2728 or click here to reach us via email. We will listen to you, explain how whistleblower rewards work, advise you on your rights, and explain your options. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.  The Cooper Health System will pay $12.6 million to settle a whistleblower lawsuit brought by one of its doctors. The suit alleged that the hospital system made improper payments to physicians for “consulting” and “advisory board” compensation in return for referrals to the hospital’s cardiology program. The physician who filed the lawsuit will receive a whistleblower reward that should be between $1.89 million and $3.15 million. The lawsuit alleged that outside physicians were paid $18,000 per year to serve on the Cooper Heart Institute Advisory Board, and that at least one purpose of these payments was to induce the physicians to refer patients to the hospital’s cardiology program. Payments by hospitals to outside physicians violate the Anti-Kickback statute and the Stark law if they are based on patient referrals. The rationale is that payments for referrals interfere with the physician-patient relationship and can lead to over-utilization and inflated costs. The law punishes both those who make the payments for referrals and those who receive the payments. A violation of the Anti-Kickback statute or Stark law also renders the resulting treatment ineligible for reimbursement from Medicare or Medicaid. Any claim for reimbursement is therefore considered a false claim. Submission of false claims to Medicare or Medicaid results in liability for treble damages, a penalty of $11,000 per claim, and in some cases criminal prosecution. In this case, a physician who was recruited to serve on the Advisory Board recognized the potential illegality and decided not to join. Instead, he filed a qui tam or whistleblower lawsuit and alerted the authorities. The qui tam provisions of state and federal False Claims Acts allow an individual to file a lawsuit on behalf of the government and share in any recovery. A qui tam lawsuit is filed initially “under seal” (in secret) and the evidence is presented only to the government. The government investigates the allegations and decides whether or not to join in the lawsuit. In this case, both the federal and state governments decided to join in the lawsuit. Cooper Health System agreed to pay $10.2 million to the United States and $2.3 million to the State of New Jersey to resolve the physician kickback and Stark law allegations without admitting wrongdoing. Under the False Claims Act, the doctor who brought the qui tam suit is entitled to a whistleblower reward of up to 25% of the amount recovered. If you are aware of hospitals, nursing homes, or other facilities that are paying physicians to serve on boards or as consultants, or providing them with low-cost office space or other benefits in return for patient referrals, then you should consult with an experienced whistleblower attorney to find out if you may qualify for a significant whistleblower reward and legal protections. The consultation is completely free and confidential. If you have a viable case, there are no attorney’s fees unless you win, in which case your whistleblower attorney will be paid out of the winnings. To arrange a free and confidential consultation, call John Howley, Esq. at (212) 601-2728 or click here to reach our offices via email. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules.  The New York Attorney General's Office recovered more than $335 million last year from companies and individuals who engaged in Medicaid fraud and abuse. New York has one of the most aggressive Medicaid Fraud Control Units (MFCU), with a staff of more than 315 people across the state. They work closely with the Medicaid Inspector General in the NYS Health Department to detect and prevent Medicaid fraud. The most common forms of Medicaid fraud in New York last year included:
The largest Medicaid fraud recoveries came from pharmaceutical companies. Abbott Labs, Boehringer-Ingelheim, Dava Pharmaceuticals, GlaxoSmithKline, K-V Pharmaceutical, McKesson, Merck, and other pharmaceutical companies paid more than $250 million to settle allegations that they submitted false price reports to Medicaid and/or promoted their products for uses not approved by the federal Food and Drug Administration (off-label marketing). Other significant recoveries involved pharmacists, hospitals, and dental clinics. Pharmacy Fraud: Four pharmacists and a pharmacy owner agreed to pay $9.9 million in restitution after pleading guilty to billing Medicaid for drugs that they never dispensed to their patients. Stark Law Violations: Cayuga Medical Center paid $3.1 million to settle a whistleblower or qui tam lawsuit alleging that the hospital billed Medicaid and Medicare for patients referred by physicians who had financial relationships with the hospital. The Stark Act prohibits a physician from referring patients to a hospital if the physician has a financial relationship with the hospital, unless an exception applies. The whistleblower in this case, a physician at the hospital, received 18% of the settlement (approximately $560,000) as his whistleblower reward. Dental Fraud: Kaleida Health repaid $1.6 million to Medicaid after an internal audit revealed that it had billed Medicaid for patients who received teeth cleanings more often than once in six months, which violated Medicaid reimbursement rules. The audit also revealed that the dental clinic had billed Medicaid for multiple visits to complete exams, x-rays, and cleanings. Medicaid regulations require dental clinics to perform and bill these tasks in one office visit. If you are under investigation or have been charged with Medicaid fraud, then you should consult with an experienced Medicaid fraud attorney immediately, before you speak with government investigators. Anything you say to the investigators can and will be used against you. To arrange a free and confidential consultation, call John Howley, Esq. at (212) 601-2728 or click here to reach our office via email. You should also consult with an experienced Medicaid and Medicare fraud lawyer if you know that your employer is submitting false claims to the government. You may be entitled to a substantial whistleblower reward and legal protections if you help the government recover money paid on false and fraudulent claims. Call our office today to schedule a free and confidential consultation. John Howley, Esq. The information you obtain at this site is not, nor is it intended to be, legal advice. You should consult an attorney for advice regarding your individual situation. I invite you to contact our law offices and welcome your calls, letters and electronic mail. Contacting us does not create an attorney-client relationship. Please do not send any confidential information to us until such time as an attorney-client relationship has been established. I practice law and offer legal services only in jurisdictions where I am properly authorized to do so. I do not seek to represent anyone in any jurisdiction where this web site does not comply with applicable laws and bar rules. |
John Howley, Esq.
350 Fifth Avenue 59FL New York, NY 10118 (212) 601-2728 |
